Gentle chiropractic care is ideal for seniors, providing safe, effective relief for aging joints. As we age, our bodies go through natural changes that affect flexibility, balance, and joint health. Many seniors live with arthritis, osteoporosis, or chronic back and neck pain that interferes with everyday activities. The good news is, pain and stiffness don’t […]
back pain
Chiropractic Care for Seniors: Gentle, Safe Relief for Aging Joints
Gentle chiropractic care is ideal for seniors, providing safe, effective relief for aging joints.

As we age, our bodies go through natural changes that affect flexibility, balance, and joint health. Many seniors live with arthritis, osteoporosis, or chronic back and neck pain that interferes with everyday activities. The good news is, pain and stiffness don’t have to be “normal” parts of aging. More older adults are discovering the benefits of gentle chiropractic care for seniors—a safe, drug-free way to improve mobility, relieve discomfort, and support healthy aging.
Why Gentle Chiropractic Care Benefits Seniors
Senior chiropractic care focuses on spinal alignment, joint mobility, and nervous system health. When the spine is moving properly, the whole body functions better. Studies show that when compared to patients who do not receive chiropractic care for non-cancer pain, patients who do receive chiropractic care are 64% less likely to be prescribed an opioid.1

Key benefits include:
- Pain relief for arthritis, back pain, and neck pain
- Improved balance and coordination, reducing fall risks
- Better posture, lowering stress on muscles and ligaments
- Increased flexibility and mobility, making daily routines easier
- Non-invasive, drug-free care, ideal for long-term wellness
For many seniors, chiropractic adjustments provide not just pain relief but also greater independence and quality of life.
Gentle Chiropractic Techniques for Older Adults
Not all adjustments are the same. At our clinic, we use gentle chiropractic techniques, which are ideal for treating seniors and their families.
Conditions Seniors Seek Chiropractic Care For
Chiropractic adjustments can help with a wide range of age-related conditions:
- Natural Pain Relief for Joints
- Arthritis and joint stiffness relief.
- Treating chronic low back pain
- Treating neck pain
- Chronic pain relief
- Headache and migraine relief
- Postural changes due to aging
By restoring spinal alignment and joint function, chiropractic care helps reduce pain while improving mobility and overall wellness.
Personalized, Senior-Friendly Care
Every older adult has unique health concerns. That’s why we tailor each treatment plan to the patient’s needs. Whether you’re dealing with osteoporosis, recovering from an injury, or simply want to stay active, our clinic provides safe chiropractic for seniors with techniques that prioritize comfort.
A Natural Path to Healthy Aging
You don’t have to accept limited mobility or chronic pain as part of getting older. With gentle chiropractic care for seniors, including the Activator Method, you can support your body’s natural healing ability, reduce dependence on medications, and enjoy more freedom in your daily life.
If you’re looking for a senior-friendly chiropractic clinic in Stuart, Florida, or searching for a gentle chiropractor near me, we’re here to help you move better, feel better, and age well.
Spinal Stenosis Treatment Options
There are many spinal stenosis treatment options you should consider before resorting to surgery. Most patients with spinal stenosis respond well to non-surgical treatments such as medication, physical therapy, and gentle chiropractic care.
Spinal stenosis is a narrowing of the spinal canal, typically caused by age, injury, or congenital disorder. The condition can cause difficulty with movement and can be debilitating. According to the American Academy of Orthopedic Surgery, spinal stenosis affects 8 to 11 percent of the population.
What is Spinal Stenosis?
Spinal stenosis is a condition where the spinal canal narrows, putting pressure on the spinal cord. Bone spurs can cause a narrowing of the spinal canal. Bone spurs are one cause of spinal stenosis. They are small bony growths that form from calcium deposits and can put pressure on the nerve roots as they exit the spine. Other causes of spinal stenosis include:
- Disc degeneration
- Spinal arthritis
- Herniated disc
- Tumor
- Osteoporosis
What Causes Spinal Stenosis?
The most common cause of spinal stenosis is osteoarthritis. It usually develops slowly over time. Most people who develop symptoms of spinal stenosis are over 50 with women at a higher risk than men.
Besides osteoarthritis, other conditions or circumstances can cause spinal stenosis:
- Narrow spinal canal
- Injury to the spine
- Spinal tumor
- Certain bone diseases
- Past surgery of the spine
- Rheumatoid arthritis
How Do Doctors Diagnose Spinal Stenosis?
Spinal stenosis is often diagnosed using diagnostic imaging. Diagnostic imaging can determine the exact location, type and extent of the problem.
What are the Symptoms of Spinal Stenosis?
The most common symptoms are pain and weakness or numbness. Stenosis can affect any part of the spine and often occurs in the lower back and neck.
Other symptoms of spinal stenosis include:
- Radiating pain
- Numbness or tingling in the arms, hands, legs, or feet
- Weakness in the extremities
- Neck pain
- Clumsiness in the arms and hands
- Abnormal reflexes
What are Non-surgical Treatments?
The majority of patients (70%) are able to manage their symptoms through nonsurgical treatments. 1
Treatments for spinal stenosis pain vary depending on the type and location of the pain. Non-surgical treatments include medication, chiropractic care, and acupuncture.
- Pain medications are prescribed to relieve the pain and reduce inflammation. Unfortunately, these medication can cause side effects.
- Gentle Chiropractic care is recommended to help relieve muscular skeletal pain. Chiropractic care improves the movement of the spine. This helps to relieve strain on the discs and nerves in the back. Gentle chiropractic care avoids the twisting, snapping and torque of traditional chiropractic adjustments.
Surgery may be recommended if non-invasive methods don’t provide symptoms relief.
Spinal stenosis is a common condition that affects millions of Americans each year. The symptoms can vary from person to person. Treatment options for spinal stenosis vary depending on how severe symptoms are and what other health conditions are present.
Acupuncture for spinal stenosis is effective for fighting the pain associated with the condition. Clinical studies 4 have shown that this holistic therapy can help relieve the types of pain caused by the condition of spinal stenosis.
Gentle chiropractic care is preferable to traditional chiropractic care for spinal stenosis.
Treatment Options for Spinal Stenosis
The most common treatment is nonsteroidal anti-inflammatory drugs (NSAIDs). NSAIDS treat pain and inflammation.
In 2007, the American Heart Association issued a scientific statement warning of the long-term use of nonsteroidal anti-inflammatory drugs (NSAIDs) 5 which included this warning:
“Consumers are advised that all over-the-counter (OTC) pain medications, including NSAIDs, should be used in strict accordance with the label directions. If use of an OTC NSAID is needed for longer than ten days, a physician should be consulted.”
If non-surgical treatments can’t provide adequate pain relief, you may need surgery. There are many kinds of surgery for spinal stenosis. The health care professionals at Advanced Wellness Solutions will help get you the care you need if they aren’t able to relieve your pain.
Call to schedule your appointment today at 772-403-7640.
Arthritis Pain Management
Gentle chiropractic is a safe, nonsurgical method of arthritis pain management. Gentle chiropractic care can help reduce inflammation and increase range of motion while reducing arthritis pain.
 Movement is like lubrication for the joints. Gentle chiropractic adjustments can help to encourage full range of joint motion to provide safe arthritis pain management. In conjunction with the gentle chiropractic adjustment, electrical muscle stimulation is often used for immediate pain relief. Patients receive appropriate exercises to perform at home to promote increased joint mobility, in addition to in-office therapies.
Movement is like lubrication for the joints. Gentle chiropractic adjustments can help to encourage full range of joint motion to provide safe arthritis pain management. In conjunction with the gentle chiropractic adjustment, electrical muscle stimulation is often used for immediate pain relief. Patients receive appropriate exercises to perform at home to promote increased joint mobility, in addition to in-office therapies.
Arthritis
Arthritis is inflammation of the cartilage, which causes swelling and tenderness in afflicted joints. Cartilage is the connective tissue that surrounds the ends of bones. It is dense, elastic tissue that supports and cushions the joints while helping joints to move smoothly. When cartilage becomes inflamed, joint pain and stiffness result.

The two most common types of arthritis are osteoarthritis and rheumatoid arthritis. While the symptoms are similar, the cause of each is dramatically different.
Rheumatoid arthritis (RA) is an autoimmune disease.
RA is an autoimmune disease that occurs when the body’s immune system attacks healthy cells by mistake. RA attacks the healthy cells in the cartilage that cushions the joints. The joints affected are usually in the hands, wrists, and knees. When the body’s immune system attacks the joint cartilage, it becomes inflamed, swollen and tender. Later, inflammation damages joint cartilage and bones. This can cause long-lasting or chronic pain, unsteadiness (lack of balance), and deformity (misshapenness). 3
Osteoarthritis (OA) is the most common form of arthritis.
OA is a degenerative condition that affects joint cartilage and bones. It causes pain, loss of mobility, as well as decreased muscle function and strength. Like RA, osteoarthritis causes joint pain and stiffness. It was once thought that in osteoarthritis, the joints were simply wearing out. Research has shown that OA is a complex process with many causes. It is not an inevitable part of aging, experts say, but rather the result of a combination of factors.
While osteoarthritis can damage any joint, it most commonly affects those that bear weight—like your knees, hips, feet, and spine. It often comes on gradually over months or years.2 Ten percent of men and 20% of women aged between 45 and 65 years report OA,4 with 80% of those older than 75 years showing radiographic evidence of OA.5
Treatments for Arthritis Pain
According to Scott Haldeman, MD, a neurologist in Santa Ana, California and Chairman Emeritus of the Research Council for the World Federation of Chiropractic, as quoted in arthritis.org6,
Chiropractic care is one of the safest therapies you can use if you have back or neck pain due to osteoarthritis.
In addition to treating neck and back pain from osteoarthritis, gentle chiropractic treatment can also treat osteoarthritis of the hip and7 other arthritic joints.
Gentle Chiropractic Care for arthritis pain

Gentle chiropractic care can help increase the range of motion in arthritic joints and reduce arthritic joint pain.
While gentle chiropractic care won’t repair or rebuild cartilage, it can relieve pressure on joints caused by arthritis. Gentle chiropractic care can also stop muscle spasms and tenderness caused by osteoarthritis through gentle manipulation of muscles and soft tissues surrounding arthritic joints.
Acupuncture for arthritis pain
For thousands of years, people have used acupuncture and Chinese medicine to relieve arthritis pain. While acupuncture can’t cure or reverse the process of arthritis, a study showed it can help you feel significantly less pain and function better. 8
Over-the-counter medications
It’s very common to reach for over-the-counter (OTC) pain medication for arthritis pain management. Regrettably, a black box warning is now attached to all NSAIDs, including OTC pain medication. The FDA reserves this, the strongest of all warnings, for drugs that pose a significant risk to the population. In 2007, the American Heart Association issued a scientific statement warning of the long-term use of nonsteroidal anti-inflammatory drugs (NSAIDs), which9 included this warning:
“Consumers are advised that all over-the-counter (OTC) pain medications, including NSAIDs, should be used in strict accordance with the label directions. Consult a physician if you need to use an OTC NSAID for more than ten days.
A practice-based study of people with both short-term and long-term low back pain found that within two weeks of care, people whose main treatment was chiropractic manipulation had significant drops in their visual analogue scale (VAS) scores.10 This study also included an evaluation of traditional medical management with primary treatment using NSAIDs. The NSAID group did not report the same level of pain reduction until the 12-week marker.
Herbs and supplements for arthritis pain relief
There are many herbal supplements that tout anti-inflammatory properties. It’s important to exercise caution when taking supplements. Just because a product is natural does not mean it’s safe. The U.S. Food and Drug Administration does not verify the contents of supplements.
Some supplements can interact with medications or can cause health problems.
You should always consult your doctor or pharmacist before taking any supplement.
Turmeric, ginger and cinnamon are supplements that reduce inflammation in the body. There is also evidence that vitamin C and fish oil may help with arthritis pain while providing other health benefits.
Glucosamine sulfate supplements have unique anti-inflammatory effects. In some laboratory tests, it demonstrated a protective effect on the cartilage as well. Chondroitin sulfate supplements also appear to have anti-inflammatory properties. Some laboratory studies suggest that chondroitin sulfate may slow cartilage breakdown associated with osteoarthritis and even stimulate cartilage growth.11
Trigger point injections for arthritis pain relief
If chiropractic treatment alone does not provide adequate pain relief, the medical professionals at Advanced Wellness Solutions may recommend a trigger-point injection. A trigger-point injection usually contains an anesthetic and a steroid to immediately help alleviate arthritis pain. These injections are rarely a standalone treatment. They work best when combined with other conservative treatment methods, such as chiropractic care.
Trigger point injection therapy can provide immediate and ongoing relief from pain in the targeted area while chiropractic treatments address the underlying cause of the pain.
Transcutaneous electrical nerve stimulation (TENS) for arthritis pain relief
Transcutaneous electrical nerve stimulation (TENS) delivers a small electric current to specific nerves. Tens units provide neuromodulation treatments that can ease pain with minimal risks and offer an alternative to pain medication for arthritis pain management. According to Arthritis.org 12
These devices are generally safe. However, they involve sending electrical impulses though your body. So it’s important to talk with your doctor first if you have a pacemaker, another implanted device, are pregnant, have epilepsy, or have a heart problem.
Topical medications for arthritis pain relief
Advanced Wellness Solutions recommends topical medications that do not contain NSAIDs.
- CryoDerm Gel: It contains almost 300% more of the active ingredient and pain reliever menthol than other topical pain relievers. Menthol is used clinically as an anti-inflammatory and pain reliever. It creates a cold sensation on the skin by activating the peripheral cold receptors.
- Biofreeze Professional: Biofreeze is greaseless, stainless and has a vanishing scent. It is an optimized, fast-acting proprietary formula.
Topical NSAIDS are now available without a prescription. Diclofenac sodium 1% gel (voltaren arthritis pain) is now available at many pharmacies. A 2016 Cochrane review concluded,14 “Topical diclofenac and topical ketoprofen can provide good levels of pain relief beyond carrier in osteoarthritis for a minority of people, but there is no evidence for other chronic painful conditions.”
Safe Arthritis Pain Management
When arthritis threatens to immobilize you, gentle chiropractic care can keep you moving.
We are currently accepting new patients. Call (772) 403-7640 to schedule your appointment.
We accept all major medical health insurance and Medicare.
You can find safe arthritis pain management at Advanced Wellness Solutions. Effective gentle chiropractic care can help to relieve the pain and slow the damage to cartilage from osteoarthritis. Gentle chiropractic maximizes the function of arthritic joints by encouraging full range of joint motion.
Gentle Chiropractic for Car Accident Injuries
Florida car accidents are happening more frequently these days. Stressed drivers are causing injury and fatality rates to climb.1 If you’ve been in a car accident, you should choose gentle chiropractic care for those injuries.
Accepting new patients. Call 855-509-5400 to schedule your appointment.
We Accept All Major Medical Health Insurance and Medicare.
Gentle Chiropractic Care for Car Accident Injuries
There are 3 Compelling Reasons to Choose Chiropractic Care after a Car Accident, When choosing a chiropractor, you’ll want to choose one that practices effective gentle chiropractic care.

Injured in a Florida car accident?
The chiropractor you choose can make a difference!

What is Gentle Chiropractic?
Many patients in pain are afraid of the traditional spinal manipulation methods. They don’t want to be twisted, snapped or “crunched.” Different chiropractic techniques and patient positioning are used to deliver effective, gentle chiropractic care. This will allows for optimal recovery after a car accident.
One gentle chiropractic modality is the Activator Method. This provides a gentle spinal manipulation for patients in severe pain. This chiropractic technique uses a small, hand-held Activator Adjusting Instrument to deliver a gentle impulse force to the spine. This gentle modality is beneficial for patients who have suffered a traumatic injury. It avoids the twisting and contortion frequently involved in traditional manual adjustment modalities.
Gentle chiropractic adjustments can to help you get back to living the life you love.
Gentle Chiropractic replaces high-velocity adjustments with low-velocity, low amplitude manipulations. There’s no twisting you into a pretzel or snapping movements.
Gentle chiropractic can treat pain in your neck, back, wrists, shoulders, hips and knees.
Gentle chiropractic care is more comfortable and provides maximum benefit from minimal visits.
Car accidents are often violent. The force of the accident places a lot of pressure on the neck and back. The neck and back are easily injured by the force. It’s no surprise that the 4 most common car accident injuries are all forms of soft tissue injuries.
- Headaches
- Neck Pain and Whiplash
- Shoulder Pain
- Back Pain
Gentle chiropractic care can prevent long-term, chronic pain conditions from developing.
If you or someone you know has been in a car accident, you need gentle chiropractic treatment. Call Advanced Wellness Solutions at 855-509-5400 to schedule an appointment.
7 Tips to Creating an Ergonomic Home Office
A lot more people are working from home these days. For many, it brings to mind images of relaxing on the couch while working. Few realize the importance of creating an ergonomic home office until they’re in pain.
On a well-known image sharing website, I searched for “working from home” and found the image below. If this is how you’ve been working from home, you may notice you have some new aches and pains. Your neck and back may be aching. Your wrists may hurt as well. Maybe you’re having headaches.
Don’t wait until you’re in severe pain to ask yourself: Is your workspace helping or hurting you? Are you working productively? Or is working from home slowly crippling you?
(By the way, this article applies to children who are homeschooling as well.)
If the decision to work from home was a sudden one, you probably didn’t give much thought to ergonomics. You set up your computer where you could and got to work.
The majority of people are unaware that an employer designed their workspace with ergonomics in mind. Ergonomics draws on many disciplines to optimize the interaction between you and the work environment. Ergonomics is how you and your workspace interact.
When your home office isn’t set up with ergonomics in mind, eventually you’ll experience:
- headaches
- shoulder pain
- back pain
- neck pain
- wrist pain, a.k.a., carpal tunnel syndrome treatment
Poor office posture injuries are repetitive use injuries.
Notice the word “eventually” above. You see, the human body is great at “making do” with whatever situation you put it in. This means the first time you flop down on your couch to work, your body isn’t going to scream at you to stop. Instead, it will do its best to adapt.
However, if you continue to put stress on your back, neck, shoulders, elbows and wrists with poor office posture, eventually you’ll experience the aches and pains described above.
It’s not just people who work from home who can suffer from these injuries. Anyone who works in an office is susceptible to these repetitive use injuries. However, if you’re working from home and you haven’t set up your home office with ergonomics in mind, then you’re even more susceptible to these types of injuries.
 Employers invest in trying to optimize workplace ergonomics because they want to increase productivity while decreasing injury and illness. According to the Bureau of Labor Statistics (BLS) in 2013, musculoskeletal disorders cases accounted for 33% of all worker injury and illness cases. 1
Employers invest in trying to optimize workplace ergonomics because they want to increase productivity while decreasing injury and illness. According to the Bureau of Labor Statistics (BLS) in 2013, musculoskeletal disorders cases accounted for 33% of all worker injury and illness cases. 1
Home Office Ergonomics Can Prevent Musculoskeletal Disorders
Work-related Musculoskeletal Disorders are among the most frequently reported causes of lost or restricted work time. These include:
- carpal tunnel syndrome (wrist pain)
- tarsal tunnel syndrome (ankle/foot pain)
- pinched nerves
- herniated disks (back/neck pain)
- tendinitis
- rotator cuff injuries (shoulder pain)
- epicondylitis (elbow pain)
- trigger finger (finger pain)
- muscle sprains, strains and tears
- mid back pain
- low back injuries
- neck pain
These Musculoskeletal Disorders have one thing in common. They all have symptoms of pain, swelling, and numbness.
 The following are frequent causes of work-related musculoskeletal disorders:
The following are frequent causes of work-related musculoskeletal disorders:
- repetitive motion involving microtasks
- overexertion
- vibrating, rubbing, or jarring.
Creating an Ergonomic Home Office
You can reduce your risk of illness or injury by keeping workspace ergonomics in mind as you set up your home office.

Create an ergonomic home office by focusing on these key elements.
#1: Choosing The Proper Chair
It’s well worth the investment to purchase a quality chair. Keep in mind you will be spending 8 to 15 hours a day sitting as you work.
Don’t let clever marketing trick you. The term “ergonomic chair” is used loosely at best and is lying at worst. Instead, focus on finding a chair that fits you properly. If you are tall or short, you may need to spend some extra time to find that perfect chair. One advantage to outfitting your home office is you can purchase the best chair for your body.
The height of the chair is paramount. You should be able to adjust your chair so your feet are flat on the floor and your legs are parallel to the floor. Tilts are helpful to get that angle just right.
The backrest of your office chair should be separate from the seat. You should also make sure you can adjust the height and angle. Be sure the chair supports the natural curve of the spine. Pay close attention to the lumbar region of the chair. Make sure your chair offers proper support in the curve of your back.
What about Exercise Ball Office Chairs? While an exercise ball is great for working out, it is not your friend as an office chair. For most people, the height of the ball is not suitable for desk work. (See the image above for proper positioning.) While it’s good to exercise your core, these exercises should only be done for a short period of time, not for an entire 8-hour workday.
#2: Choosing the Proper Keyboard/Mouse
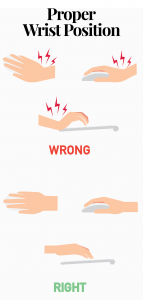 Many office workers suffer from tendinitis, carpal tunnel syndrome and other repetitive strain injuries caused by poorly designed keyboards and mice or positioning.
Many office workers suffer from tendinitis, carpal tunnel syndrome and other repetitive strain injuries caused by poorly designed keyboards and mice or positioning.
Finding the right keyboard and mouse is difficult because there is no “one size fits all” product or solution. While there’s no one product that is right for everyone, there are things to keep in mind to help you find the perfect match!
- Distance: Proper sitting posture dictates where you should place your keyboard.
- Angle: The keyboard should have a slight negative angle of about 15 degrees
- Height: Your posture and desk height dictate the correct height of your keyboard and mouse
- Mouse: the most important thing is to make sure you don’t twist your wrist while using the mouse
What about Wrist rests?
Often a wrist rest is used as a support rather than a rest. It should only be used, ideally, when a sharp or hard surface is present that you are constantly coming into contact.
#3 Laptop: Ergonomic Friend or Foe
Unfortunately, your laptop is an ergonomic foe! Laptop computers are much more convenient and portable than desktop varieties. However, it’s the ability to use your laptop anywhere that makes it an ergonomic foe! Using it while in bed or while seated on the sofa is a recipe for neck, shoulder and back pain. In addition, the keyboard is flat, which means your wrists won’t be properly positioned.
If you must use a laptop computer, don’t use the laptop’s keyboard and mouse pad. Instead, purchase an ergonomic keyboard and mouse and attach them to your laptop just as you would to a desktop. Place the laptop on a flat surface and position the screen to the proper height. See the illustration above. When you do this, you will find it very uncomfortable to use the laptop’s keyboard/mouse.
#4: Using the Phone
Do Not Cradle Your Phone!
If you are on the phone and typing, cradling the phone between your ear and shoulder can be hazardous to your neck. Cradling the phone can lead to neck spasm, headaches and ear pain.
Using speakerphone is the fastest and easiest solution. If using your phone’s speakerphone isn’t an option, invest in a good headset. It will literally save your neck!
#5: Choosing a Desk
Height is by far most important factor in choosing a desk for your ergonomic home office. The Canadian Standards Association (CSA) recommends a general height desk of 28.7 plus or minus 1.
Many people work from home from their dining table. Standard dining table heights are 28″ – 30 so it’s possible your dining table is the proper desk height. It’s also possible that your dining table is just a bit too tall or short. In the Work From Home Office Ergonomics illustration above, make sure your arm rest allows your elbow to be at a 90° angle while working at your table. If not, shoulder, wrist, neck and back pain can result.
#6: Positioning Your Monitor
- Distance: Your monitor should be set up 20 inches away or at arm’s length
- Elevation: The top of the screen should be at or slightly below eye level. The monitor should be directly behind your keyboard. If you wear bifocals, lower the monitor an additional 1 to 2 inches for more comfortable viewing.Tilting your head back to try to read your monitor can lead to headaches and neck pain.
- Angle: 10-20 degrees A greater angle will cause you to hold your head at an uncomfortable angle, leading to neck strain.
- Glare: Glare on your screen causes eye strain. Placing your monitor and desk perpendicular to the window works best. Whatever kind of lighting you use, position the monitor so that there is no distracting glare.
#7: Footrest
Footrests are a way to shift postures or provide support for the feet if the chair cannot be lowered. Unfortunately, using a footrest when the chair is too high provides only one place for the feet to rest.
- Height: Footrests should be adjustable. Adjust the footrest until the thighs are parallel to the floor +/- 1-3 inches.
- Rocking: When using a footrest, be sure to shift postures frequently. The rocking action on all-plastic footrests tends to wear out quickly, so look for durable models.
Chiropractic Care Can Help!
If you haven’t set up an ergonomic home office, you may already be feeling the effects. Sometimes simply changing your workspace can help alleviate your pain. If it doesn’t, gentle chiropractic care can help. Chiropractic care focuses on treating all of your joints and muscles. If you work on a computer all day, be sure to ask Dr. Danielle about adjusting your wrist.
Sleep is Important for Health
Sleep is important for health and well-being. According to the NIH, sleep is essential for vital bodily functions such as growth and development, energy conservation, brain waste clearance, modulation of immune responses, cognition, performance, vigilance, disease, and psychological state. Sleep is also critically important to healing from injuries. Chronic pain is just one of many conditions that can keep you from getting the healthy sleep you need.

If you have trouble sleeping, you’re not alone. The American Sleep Association reports that nearly one-third of adults don’t get the recommended 7 hours of sleep each night, and sleep quality is declining.
Though the exact mechanisms are not fully understood, the current research suggests that individuals with a sleep disorder may be more likely to develop chronic pain, and people with chronic pain are more likely to have trouble sleeping.1
A growing body of evidence suggests that sleep problems pose an important risk for the development of musculoskeletal pain in adolescents. A large cross-sectional study involving 6986 adolescents found short sleep time to be a risk factor associated with regional musculoskeletal pain, particularly chronic regional pain and chronic widespread pain.2
Why Sleep is Important for Health
When you crawl into bed to go to sleep, you might think your body is shutting down and resting. We now know nothing could be further from the truth. Sleepy time is when your body performs many “heavy lifting” tasks that repair, restore and maintain your mind, body and health. These processes are so intensive that the body waits until you’re asleep to perform them. This is why getting proper sleep following surgery or an injury is an important part of the healing process.
If you’ve been injured in a car wreck or suffer from chronic pain, getting that healthy sleep is easier said than done.

Sleep is Important for Health & Injury Recovery
While sleep is important for health, it plays a surprisingly important role in injury recovery. Whether you’ve been in a car accident or you’ve hurt yourself at work or play, you need to get healthy sleep so your body can repair damage to muscles, ligaments, tendons, and even bones.3
According to John DeLucchi, physical therapy manager for OrthoCarolina, “If you want to upgrade your athleticism, decrease your risk of injury, decrease persistent pain, recover faster, boost your immune system, have more energy and perform better, sleep is critical.” 4
Your immune system relies on sleep to be able to fight harmful substances. When you don’t get enough sleep, your immune system can’t properly protect your body from infection. Your body makes white blood cells while you sleep. These white blood cells attack viruses and bacteria that can slow the healing process as well as make you sick.

Sleep is when the body manufactures hormones. During healthy sleep cycles, the brain triggers the release of hormones that encourage tissue growth to repair blood vessels. This process helps wounds to heal faster and restores sore or damaged muscles. Some of the hormones your body makes and releases during sleep slow breathing and relax muscles. This process can reduce inflammation and assist with healing. Other hormones your body releases are the ones that make you feel hungry or full. When you don’t get enough sleep, the hormone levels of ghrelin go up. Ghrelin is called the ‘hunger hormone’ because it stimulates appetite, increases food intake and promotes fat storage. 5At the same time, the hormones that tell your body that you’re full (leptin) go down. 4This is why poor sleep patterns often lead to overeating and obesity.
 So, to recap, healthy sleep helps you
So, to recap, healthy sleep helps you
- heal and recover after surgery or injury
- relax muscles
- repair blood vessels
- fight infection
- restore sore and damaged muscles
- maintain a healthy weight
In a cruel catch-22, chronic pain sufferers find it difficult to get healthy sleep. Chronic pain can lead to sleep disturbances, depression and a heightened risk of suicide. 5 Healthy sleep plays a vital role in battling chronic pain, but chronic pain often prevents healthy sleep patterns.

Good Sleep Hygiene
Here are some things to try to help you get a healthy night’s sleep.
-
- Make your bedroom a sleep sanctuary. Reserve the bedroom for sleep, intimacy, and other restful activities.
- Keep your bedroom cool. Between 60 and 67 degrees Fahrenheit for optimal sleep.6
- Banish electronics from your bedroom.
- Be careful about napping. Taking a nap at the peak of sleepiness in the afternoon can help to supplement hours missed at night. However, daytime naps can also interfere with your ability to sleep at night.
- Instead of napping, try taking a brisk walk. Exercising—especially when you’re having trouble sleeping—is tough but worth the effort. Make sure to avoid exercising within three hours of bedtime.
- Avoid caffeine after noon.
- Alcohol is not a sleep aid. While many people think drinking alcohol helps you sleep, studies show the opposite is true. 7While alcohol will make you fall asleep faster, the quality of sleep you get is greatly diminished. The more you drink and the closer your drinking is to bedtime, the more it will negatively impact the quality of your sleep.
If you’re having trouble sleeping, it’s time to schedule an appointment with Advanced Wellness Solutions. Acupuncture has been used for thousands of years to:
- Reduce depression and anxiety 7
- Improved sleep quality, sleep efficiency and total sleep time8
- Increase energy and improve fatigue9
Call (772) 403-7640 to schedule your appointment.
Chiropractic Treatment for Disc Herniation
Chiropractic treatment is a non-surgical option for disc herniation. Chiropractic care is frequently the preferred first choice for treatment since it is non-invasive and avoids the use of medications or injections.
 Your spine is made up of a series of bones (vertebrae). Between each bone is a rubbery disc that acts as a cushion. When the soft center of a rubbery disc is pushing through a crack in the tougher exterior casing, it’s called a disc herniation.
Your spine is made up of a series of bones (vertebrae). Between each bone is a rubbery disc that acts as a cushion. When the soft center of a rubbery disc is pushing through a crack in the tougher exterior casing, it’s called a disc herniation.
With proper treatment, a herniated disc does not mean a lifetime of unbearable pain.
Is a herniated disc serious? Yes. Many herniated discs can be managed successfully with proper care and monitoring.
Seek immediate medical attention if you have:
- Loss of balance, bladder control or consciousness
- Vomiting
- Loss of sensation
- Symptoms are rapidly getting worse
A disc herniation falls into a broader category of disc derangement.
Disc derangement is a general term for when a disc has been damaged. This damage can be minor or major depending on age and type of trauma. The disc is made up of a gelatinous center called the nucleus pulposus surrounded by fibrocartilaginous material (annulus fibrosis). When the annulus fibrosus is torn due to stress, the gelatinous nucleus pulposus can ooze out.

How far that gelatinous nucleus pulposus oozes out is what determines what kind of disc derangement you have.
There are four stages of disc derangement:
- degeneration,
- prolapse,
- extrusion,
- and sequestration.
Degeneration
The first stage of disc derangement is when the nucleus pulposus begins oozing into the layers of annulus fibrosis.
Prolapse
Prolapse is when the nucleus pulposus pushes all the way out to the last layers of the annulus.
Extrusion
Extrusion is when nucleus pulposus has left the confinement of the annulus fibrosis. This is the state where nucleus pulposus can physically start interfering with surrounding structures.
Sequestration
Sequestration is the most severe. The nucleus pulposus has left the confinement of the annular fibrosis and has broken off into little pieces. These pieces can travel and cause interference with the surrounding structures.

Any stage of disc derangement can cause pain.
How much pain depends upon the individual and the location of the derangement. Extrusion and sequestration pose the most serious risk of the four. Anytime nucleus pulposus has left its confinement, it can cause impingement and pain.
In rare cases, disc derangement actually pinches a nerve, causing pain. Usually, the pain associated with disc derangement comes from the inflammatory response of the body to the change in structure. Inflammation occurs around the deranged disc, causing the nerve to become irritated. This in turn causes pain.
An MRI can show the location and what type of disc derangement is present.
What are the symptoms of a herniated disc?
Disc issues can manifest in various forms. Some individuals may have herniated discs yet experience no noticeable symptoms. The nature of the symptoms varies based upon where the herniated disc is located.
Cervical disc herniation symptoms:
- Pain in the arm or hand; this pain often feels like it is traveling down the arm or radiating
- Numbness and tingling
- Weakness in the arms
- In severe cases, reduced reflexes in the upper limbs with increased reflexes in the lower limbs
Lumbar disc herniation symptoms:
- Low back pain that travels down the buttocks, legs and feet
- Numbness and tingling
- Weakness in the legs
- Decreased reflexes
Risk factors for herniated disc:
- Overweight: excess weight puts extra stress and different weight loading on discs
- Physically demanding jobs
- Genetics: a family history of disc herniation
- Age: most likely to occur between 30 and 50
What causes a herniated disc?
Herniated discs can happen gradually with repeat stress. In other cases, trauma (like a car accident) can damage or displace one or more discs.
Common car accident injuries include
- bulging discs (when a disc shifts out of place and bulges into the spinal canal),
- annular tears,
- herniated discs.
How do you treat a herniated disc?
Treatments for a herniated disc include:
- Gentle chiropractic treatment with adjustments
- Acupuncture
- Medical massage therapy
- Cervical traction
- Physical therapy
- At-home exercises and stretches
- Postural correction
- Weight reduction
- OTC pain medications, muscle relaxers and prescription opioids.
- Surgery
An important thing to remember with a herniated disc is to avoid too much bed rest. Lying in bed waiting for the pain to go away is one of the worst things you can do. Taking it easy and not lifting heavy things is fine.
Gentle Chiropractic Treatment for Disc Herniation
Gentle chiropractic care has been demonstrated to effectively treat lumbar disc herniation. A gentle chiropractic care technique (activator method) has advantages over traditional chiropractic techniques when treating symptomatic lumbar disc herniation.1
We [the case study authors] speculate that the use of an AAI, combined with Activator methods, may provide definitive benefits over side-posture manipulation of the lumbar spine in treatment of resistive disc lesions, because of the lack of torsional stress imposed upon the disc during instrumental spinal adjustment.
In another case study, Activator-assisted spinal manipulative therapy had positive subjective and objective results for low back pain in a patient with degenerative disk disease.2
Yet another case study concluded:3
Conservative chiropractic treatment may provide an effective therapeutic intervention in selected cases of cervical disc protrusion.
This study specifically cited “instrument-delivered adjustments” (gentle chiropractic) as providing benefit in cases in which manual manipulation causes an exacerbation of the symptoms or is contraindicated altogether.
Other gentle chiropractic techniques, such as the flexion-distraction technique, the drop technique and pelvic blocking, have been shown to be helpful in treating disc herniations.3,4
Flexion-Distraction Technique

This spinal adjustment method utilizes a specialized table that allows the chiropractor to gently stretch your spine.

The photo above is of William sitting on our specialized table that gently stretches your spine.
This technique is gentle and typically painless, making it suitable for individuals experiencing significant discomfort. It can help reposition the herniated disc away from the nerve, providing symptom relief.
Pelvic blockage Treatments
This approach makes use of specially designed cushion wedges. During treatment, these wedges are placed beneath each side of your pelvis. This positioning helps to naturally shift the herniated disc away from the impacted nerve. In addition to addressing herniated discs, pelvic blocking can also be beneficial for other issues such as headaches and general body pain.
Acupuncture Treatment for Disc Herniation
Herniated discs can cause inflammation and pain, but acupuncture can reduce it. While it doesn’t address the root cause of degenerative disc disease, acupuncture can provide relief from symptoms and help slow the disease’s advancement.
Individuals undergoing acupuncture treatment could see a faster healing journey. Additionally, acupuncture aids in improving overall movement capabilities. When it comes to alleviating pain and enhancing mobility, acupuncture may offer more advantages compared to traditional physical therapy methods. After undergoing surgery for a lumbar disc issue, acupuncture might prove to be more beneficial than standard medical treatments for alleviating post-surgical discomfort.
Medical Massage Therapy Treatment for Disc Herniation
- enhances blood flow to the affected region
- aids in regaining mobility in the joints,
- and provides support to the herniated area.
Medical massage therapy may boost the likelihood of natural healing for the disc, potentially facilitating the disc’s return to its proper position.
If you are experiencing symptoms of a herniated disc or have been in a Florida car accident and fear you have a herniated disc, you should contact Advanced Wellness Solutions.
Chiropractic Treatment of Poor Posture and Text Neck
Chiropractic treatment of poor posture and text neck is an effective approach for addressing both acute and chronic pain. 1
As the use of computers, long-distance driving, and mobile phone usage increases, maintaining proper posture becomes crucial. When individuals sustain poor posture over extended periods, they can develop postural syndrome, or postural dysfunction, leading to discomfort.

What is postural syndrome?
Postural syndrome is the result of prolonged time in poor posture. This posture includes head forward, shoulders slouched and the upper back arched for the upper body. For the lower body, poor posture is slouched forward while sitting or with the hips pushed forward when standing. This posture causes the muscles in the front of the body to become tight and the muscles in the back of the body to become stretched and weak. This poor posture can occur in many aspects of life, such as at the computer, gardening or cleaning.
If you are spending a large amount of your time with your arms stretched out in front of you (for example, holding your phone), then you are in a position that could lead to postural syndrome, a.k.a. text neck.
What are the symptoms of postural syndrome?
The symptoms of postural syndrome most often occur while the person is holding the problem position for extended periods of time. These symptoms are:
- Pain when the muscles of the upper back are pressed on
- Forward head carriage
- Muscle tightness
- Dull aching pain
- Burning pain in the upper back all the way up to the base of the head
- Headaches
- Muscle fatigue
How do you treat postural syndrome?
Chiropractic treatment of poor posture and text neck is an effective approach for addressing both acute and chronic pain.
- Gentle chiropractic
- Acupuncture
- Medical massage therapy
- Physical therapy
- Postural Taping
- Postural Exercises
- At home strengthening exercises and stretches
- TENS unit
- Ergonomic corrections
A key with postural syndrome is being aware of one’s posture; this is where postural taping is helpful.
If you are experiencing poor posture or symptoms of postural syndrome and wish to discuss your treatment options, please schedule your appointment by calling 855-509-5400.



